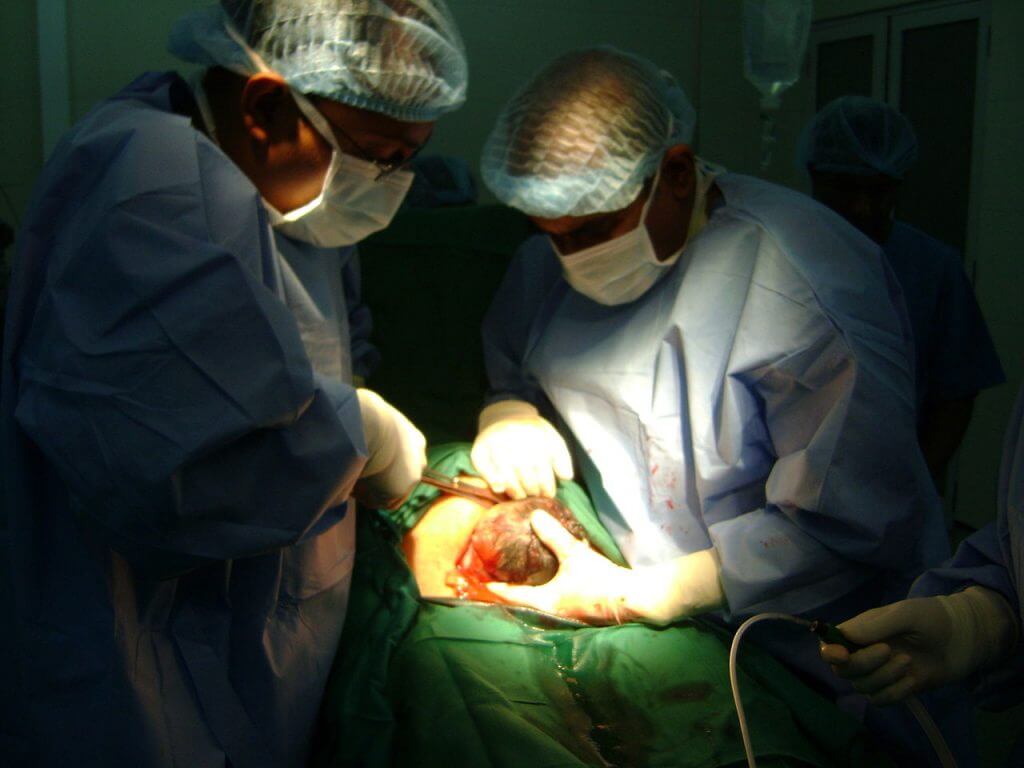
A Caesarean or C-section is the surgical method of delivering one or more babies. In this method of delivery a baby using a surgical incision in the mother’s lower abdomen and also the uterus. There are cases when a C-section is scheduled in advance when there are any known complications. But in other cases, it’s done when an unexpected complication arises. It may be done with a spinal block such that the woman is awake and be with her newborn soon afterwards or under general anaesthesia. A urinary catheter is used to drain the bladder, and the skin of the abdomen is then sterilised. In low-risk pregnancies, there is a small increase in an adverse outcome with a C-section. They also typically take longer to heal from, about six weeks, than vaginal birth. According to the U.S. Centers for Disease Control, about 33 percent of American women who gave birth in 2011 had a cesarian delivery.

The possibility of a C-section cannot be entirely ruled out no matter what type of birth plan you have or hope to have. A C-section need not always be a negative experience whether you are prepared for it or not. Most pregnant women have natural and normal delivery of the baby through vaginal birth or (birth canal). But in some cases, a C-section is required for the safety of the mother and baby.

In certain conditions, the need for a c-section for delivery is known even before a woman goes into labour. A C-section is required in cases where:
If problems arise that make it dangerous to you or your baby by continuing normal delivery or inducing labor in the following cases:

First, your practitioner will explain why he believes a c-section is necessary, and you’ll be asked to sign a consent form.
An anesthesiologist will then come by to review various pain-management options. An epidural or spinal block will be given that will numb the lower half of your body. However, you will be awake and alert for the birth of your baby.
A catheter will be inserted into your urethra, and this helps to drain urine during the procedure. An IV will be started if you don’t have one inserted already. They will remove some of the pubic hair, and you will be moved into an operating room. You may be given an antacid medication to drink before the surgery as a precautionary measure if an emergency arises for general anaesthesia. You’ll probably be given antibiotics through your IV to help prevent infection after the operation.
C-section is not a very risky procedure, and in most cases, both the mother and the baby (or babies) will be healthy and fine. However, it is a major abdominal surgery, and so it is comparatively riskier than the natural vaginal delivery. Some women develop an infection after their c-section. Other complications such as more postpartum pain, excessive bleeding, a longer hospital stay, blood clots and a longer recovery. Injuries to the bladder or bowel, although very rare, are also more common.
It is the most powerful creation to have life growing inside of you.There is no bigger gift